Home » Products » Ortho-biologics » ORTHOPLASTY™

ORTHOPLASTY™
Subchondral bone plasty (BMLs) treatment kit
- Safe and precise minimally-invasive percutaneous approach;
- Fast procedure: approximately 20 minutes procedure;
- Rapid functional recovery;
- Pain relief after 1 day;
- Preservation of anatomical physiology for future operations;
- Reduced risk of infections;
- Ready-to-use bone substitute:
– No preparation needed;
– Hardening in the wet environment only: no time pressure during application;
– Truly biologic: composed of a microcrystalline, calcium-deficient hydroxyapatite (major bone constituent);
– High compressive strength (up to 45 MPa);
– Radio-opaque paste: clearly visible under fluoroscopy and X-rays;
– Bioresorbable during bone remodelling.
ORTHOPLASTY™ is a minimally invasive, fluoroscopically guided procedure designed to identify and treat subchondral bone defects, also known as Bone Marrow Lesions (BMLs). This technique can be combined with arthroscopy for simultaneous intra-articular monitoring.
The pathology is generally classified as Subchondral Insufficiency Fracture of the Knee (SIFK) or Spontaneous Osteonecrosis of the Knee (SONK). Patients typically present with intense pain despite mild radiographic changes, often associated with early osteoarthritis. As these lesions are not visible on X-rays, MRI is required for diagnosis, revealing hyperintense signals in T2-weighted and STIR sequences due to fluid accumulation.
The goal of subchondral bone plasty is to reinforce subchondral bone using principles similar to vertebroplasty. The procedure involves percutaneous insertion of a bone substitute or an autologous bone graft, often enriched with mesenchymal stromal cell concentrate, directly into the site of bone rarefaction to restore structural integrity and improve patient outcomes.
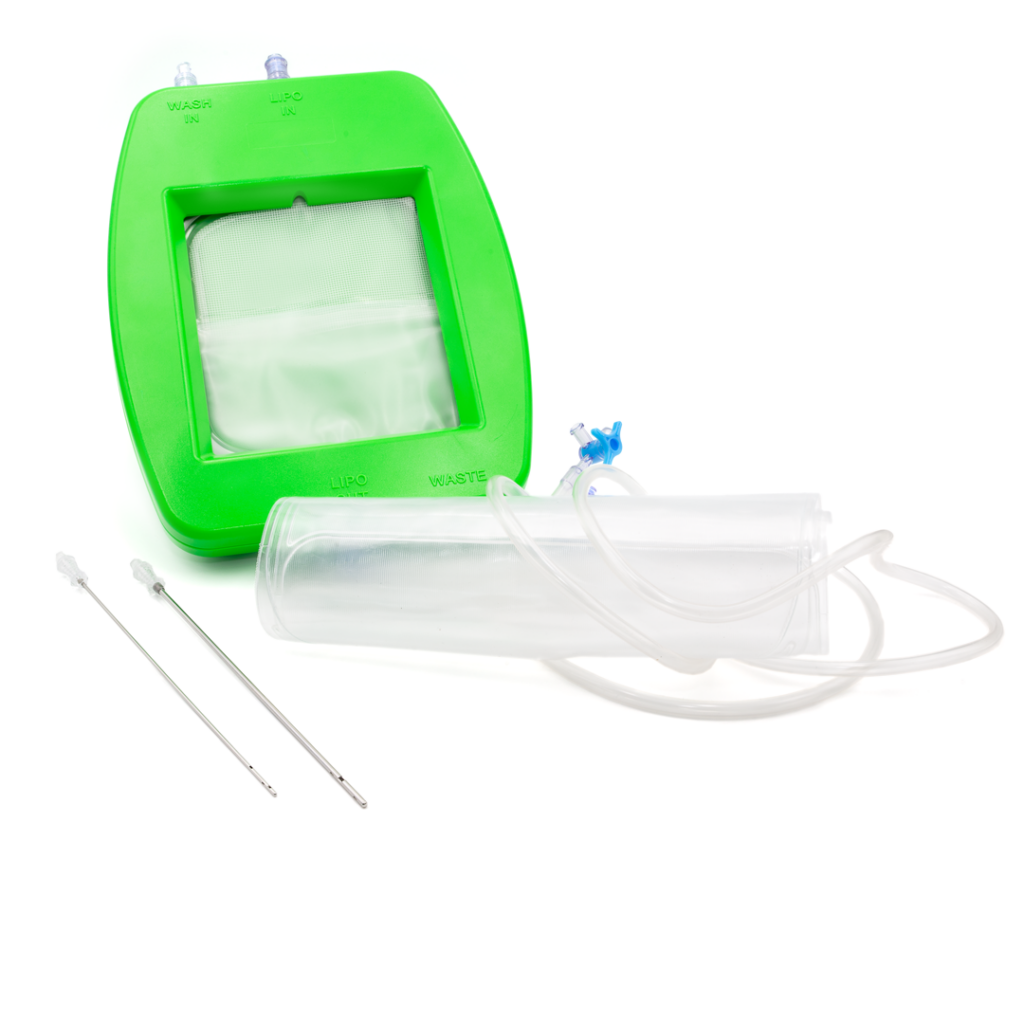
ORTHOPLASTY™ kit order codes:
- SUB1110C includes 1 trocar working cannula, 1 drill, 3 directable bone fillers, and 3 syringes (2,5 ml).
- SUB1110C-01 includes 1 trocar working cannula, 1 drill, 3 directable bone fillers, 3 syringes (2,5 ml), and biological cement.