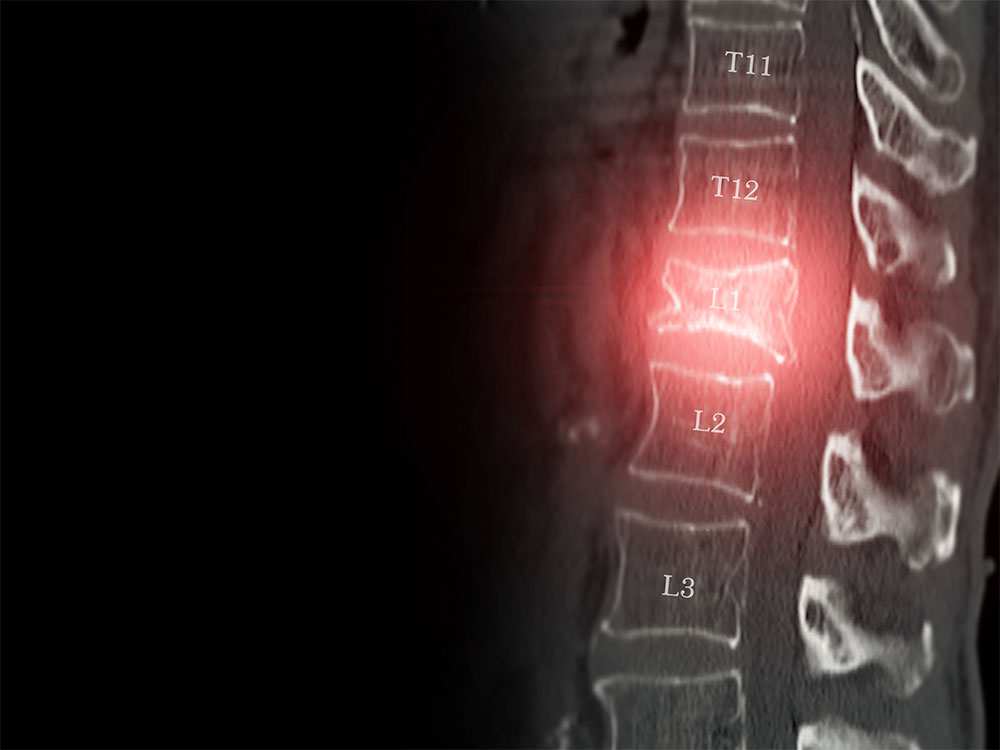
The burden of vertebral fractures
The progressive ageing of the population has made the need for rapid, minimally invasive interventions increasingly central. For elderly patients, avoiding prolonged and high-risk periods of bed rest is not only a clinical choice but a vital priority.
Within this context, two key procedures for treating vertebral fractures have gained widespread acceptance in recent years: vertebroplasty and kyphoplasty.
Vertebral compression fractures (VCFs), often associated with osteoporosis, are not merely a source of acute pain; they represent a direct threat to patient independence.
At Biopsybell, we are well aware that each day of immobilisation increases the risk of secondary complications. These are not only physical in nature, but also psychological: the sense of helplessness and isolation linked to prolonged bed rest may contribute to a rapid cognitive decline and a reduction in emotional well-being.
Fortunately, interventional medicine today offers effective, targeted and clinically established solutions.
Vertebroplasty vs kyphoplasty: what are the differences?
It is essential to clearly understand the technologies available to the surgeon:
Vertebroplasty
This procedure involves the percutaneous injection of bone cement (PMMA) into the fractured vertebral body, with the aim of stabilising the vertebra and reducing pain.Kyphoplasty
This technique involves the insertion of a balloon, which, once inflated, aims to partially restore vertebral height before the infusion of bone cement.
The benefits of the minimally invasive approach
Why should a patient opt for these procedures instead of conservative treatment based on bracing and prolonged rest?
Rapid pain relief
Most patients experience significant pain reduction within the first 24–48 hours.Return to daily activities
Restoring mobility helps prevent pressure ulcers and muscle mass loss and contributes to preserving psychological well-being, reducing the emotional impact associated with loss of independence.Day Hospital procedure
Often performed under local anaesthesia or light sedation, these techniques minimise surgical stress and support a faster recovery.
Safety first: the excellence of Biopsybell materials
The success of a vertebral stabilisation procedure is closely linked to the quality of the instrumentation used. Biopsybell kits are designed to provide clinicians with excellent ergonomics and precise control over injection pressure. In addition, our bone cement ensures optimal viscosity and radiopacity, technical parameters that translate into a high level of safety for both surgeon and patient.
Conclusion
Chronic pain and immobility no longer need to be accepted as inevitable consequences of ageing. The synergy between minimally invasive surgery and high-precision medical devices makes the return to an active life a tangible goal. Restoring movement ultimately means restoring dignity, autonomy and quality of life for our elderly patients.